How Do We Diagnose a Detached Retina Retinal detachments can usually be seen when a veterinary ophthalmologist examines the back of the eye with an instrument called an ophthalmoscope. In this study, cats with presumed congenital/juvenile cataracts who underwent phacoemulsification had an excellent outcome. In older cats the most likely cause of retinal detachment is elevated blood pressure. Twenty-one out of 22 eyes had a successful outcome. Success was defined as a comfortable and visual eye without intraocular neoplasia, glaucoma, a partial or complete retinal detachment, or uveitis that occurred >2 wk after surgery or persisted longer than 2 wk. All eyes remained visual at last follow-up (range: 0.5–121 mo). No eyes had developed intraocular sarcomas at the time of their last exam. My experience is this: if retinal detachment is detected while the retina is only partly peeled away, it will reattach once the blood pressure is controlled. You can see a widely dilated yellow pupil, and the greenish bulging retina in the middle. Recorded complications were 3 eyes developed postoperative ocular hypertension, 1 eye developed glaucoma, 7 eyes developed feline herpes virus-1 signs, and 7 eyes developed postoperative uveitis >2 wk after surgery. The picture shows a severe case of retinal detachment. The median age at the time of surgery was 15 mo (range: 4.5–168 mo of age). This retrospective study spanned 13 yr and involved 22 eyes. 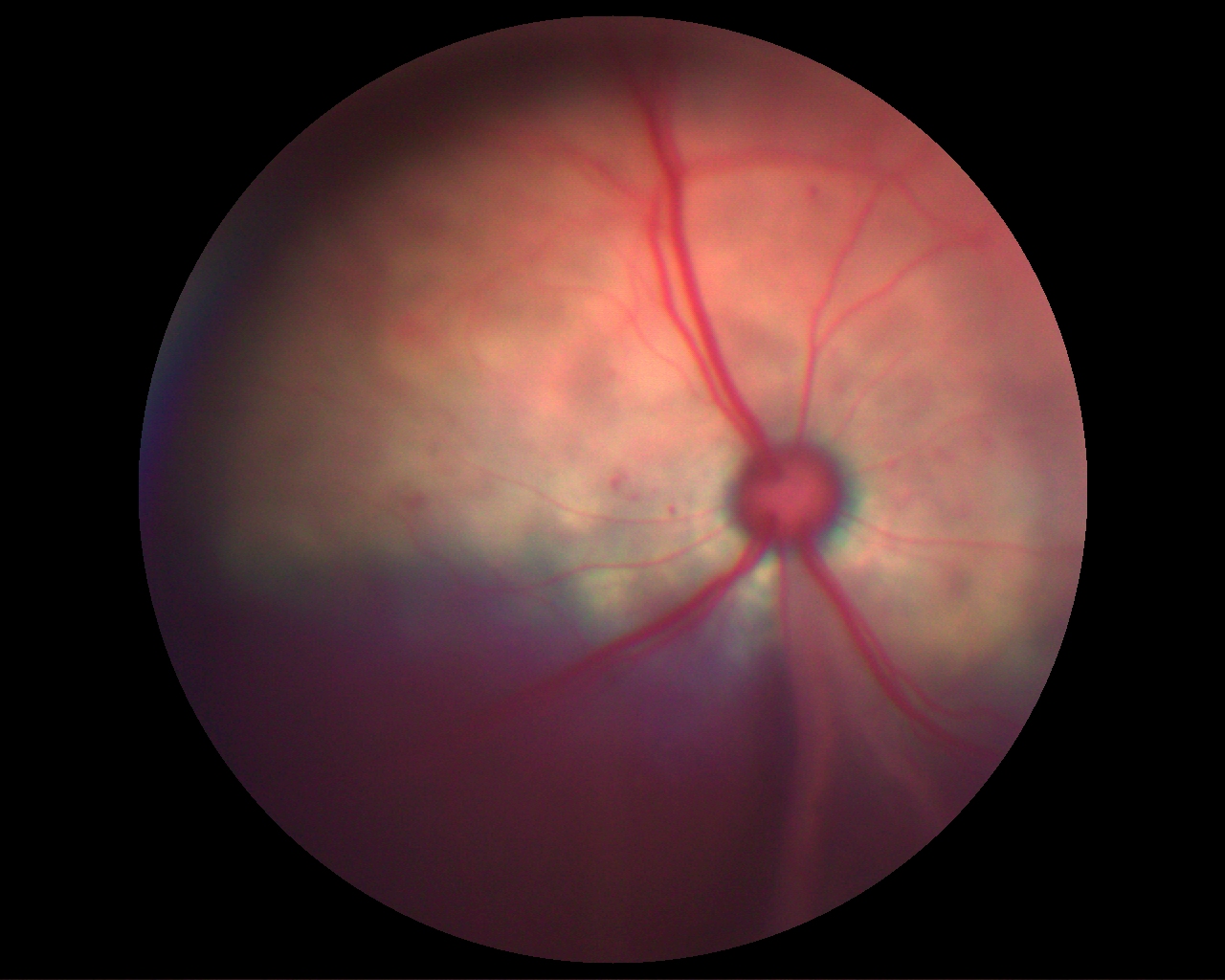 
Twelve client-owned cats were included in the study. There is a large bullous retinal detachment medial to the optic nerve head and focal areas of retinal oedema lateral to the optic nerve head. The objective of this study was to determine the complication risk and prevalence after phacoemulsification in cats with presumed congenital/inherited cataracts.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
